When a patient walks into an emergency room and can’t communicate their symptoms to the doctor treating them, the stakes couldn’t be higher. A missed detail, an allergy, a chronic condition, a medication interaction, can mean the difference between effective treatment and a life-threatening error. This is exactly the problem medical interpreting solves. The medical interpreting definition centers on a trained professional facilitating spoken communication between a healthcare provider and a patient who don’t share a common language, ensuring accuracy, clarity, and cultural understanding in every clinical interaction.
It’s a role that gets confused with medical translation far more often than it should. Translation deals with written documents; interpreting happens in real time, face-to-face or through remote technology, during appointments, procedures, and consultations. The distinction matters because the skill sets, certifications, and situational demands are fundamentally different. Understanding what medical interpreting actually involves, and what it requires, helps healthcare organizations make better decisions about how they serve multilingual patient populations.
At Languages Unlimited, we’ve provided professional interpretation services across all 50 states since 1994, including on-site, telephonic, and video remote interpreting for hospitals, clinics, and healthcare systems nationwide. This article breaks down the full scope of medical interpreting: what it means, where it’s used, who performs it, and the standards that govern it, so you can approach these services with a clear understanding of what’s involved.
Why medical interpreting matters
The United States is home to over 67 million people who speak a language other than English at home, according to U.S. Census Bureau data. A significant portion of those individuals are classified as limited English proficient (LEP), meaning they cannot communicate in English well enough to navigate complex environments like healthcare settings without support. When those individuals seek medical care, the quality of the communication they receive directly shapes the quality of the care they get.
The patient safety impact
Medical errors tied to communication failures are among the most preventable problems in healthcare. Studies have consistently shown that LEP patients who receive professional interpreter services experience outcomes comparable to English-speaking patients, while those who rely on ad hoc interpreters, such as family members or untrained bilingual staff, face significantly higher rates of medical errors and harmful misunderstandings. A child interpreting for a parent during a cancer diagnosis, or a bilingual receptionist pulled in to explain a procedure, puts both the patient and the provider in a difficult position.
When a healthcare provider works with a trained medical interpreter, the accuracy of clinical communication improves, and patient outcomes follow.
Professional interpreters are trained to deliver complete, accurate, and impartial interpretations, covering medical terminology, dosage instructions, verbally explained consent forms, and sensitive diagnoses. That level of precision is not something an untrained bilingual person can reliably produce under pressure, no matter how fluent they are in both languages.
The legal and compliance obligations
Beyond patient safety, healthcare organizations in the United States carry clear legal obligations to provide language access services to LEP individuals. Title VI of the Civil Rights Act of 1964 prohibits discrimination based on national origin by any program or activity receiving federal financial assistance, which covers most hospitals and clinics. The Department of Health and Human Services has reinforced this through guidance that requires meaningful access to language services for all patients, regardless of their language background.
For organizations covered by Section 1557 of the Affordable Care Act, those obligations extend further, reaching specific requirements around interpreter qualifications and service availability. Grasping the full medical interpreting definition helps your organization recognize this not as a compliance checkbox, but as a core part of delivering equitable, high-quality care to every patient who walks through your doors.
Medical interpreting vs medical translation
The two terms get used interchangeably far too often, but they describe fundamentally different services. Medical translation involves converting written documents from one language to another, such as patient intake forms, discharge summaries, consent paperwork, or clinical study materials. A translator works with text, typically with time to research terminology and review the final product before it reaches anyone.

How delivery sets them apart
Medical interpreting, by contrast, operates entirely in spoken or signed language in real time. When a doctor explains a treatment plan to a patient who speaks Somali, or when a nurse walks a Mandarin-speaking patient through post-surgical care instructions, no written document changes hands. The interpreter listens, processes, and conveys the message immediately, with no opportunity to pause and consult a reference. This live, spoken nature is central to any accurate medical interpreting definition: it is a real-time communication service, not a document service.
The format difference means you cannot substitute one for the other. A translated consent form does not replace an interpreted conversation during a procedure.
Why this affects your service decisions
Your organization needs both services, but for different situations and different workflows. When a patient needs to sign a consent form and asks what a specific term means, you need an interpreter available, on-site, by phone, or via video. When you need to update your patient-facing intake materials for Arabic-speaking populations, you need a qualified medical translator handling that document work separately. Treating the two as interchangeable creates gaps in care, where providers assume a translated brochure covers the communication needs of a live appointment that it cannot. Knowing which service applies to which situation helps you build a language access plan that holds up under real clinical conditions.
What a medical interpreter does
A medical interpreter’s job extends well beyond swapping words from one language to another. They accurately convey the full meaning of everything spoken during a clinical encounter, including tone, nuance, and intent, so that both the provider and the patient walk away with the same understanding. This is the operational core of the medical interpreting definition: real-time, accurate, and complete spoken communication between two parties who cannot communicate directly.
Core responsibilities
During an appointment, a medical interpreter renders every word spoken by the provider and the patient, including questions, answers, diagnoses, instructions, and emotional expressions. They do not summarize, omit, or editorialize. If a patient says they feel "like something is squeezing my chest," the interpreter conveys that description precisely, not a sanitized paraphrase of it.
Accuracy in medical interpreting means rendering the message completely, not just the parts that seem clinically relevant.
Medical interpreters also handle specialized terminology without slowing down the interaction. They know how to interpret terms like "myocardial infarction," "contraindication," or "informed consent" in ways that remain both accurate for the provider and understandable for the patient, adjusting register without changing meaning.
Professional standards interpreters follow
Qualified medical interpreters follow strict codes of ethics that govern confidentiality, impartiality, and accuracy. They do not share patient information outside the encounter, they do not advocate for either party, and they signal clearly when clarification is needed rather than guessing. Your interpreter should be trained to these standards, not simply fluent in two languages.
Healthcare organizations relying on certified or qualified interpreters reduce liability exposure and demonstrate compliance with federal language access requirements. Fluency alone does not qualify someone for this role.
Where medical interpreting happens
Medical interpreting takes place across a wide range of healthcare environments, from emergency departments to routine outpatient appointments. The core medical interpreting definition holds regardless of the setting: a trained professional bridges spoken communication between a provider and a patient in real time. Understanding where these services apply helps you identify exactly where your organization needs coverage and which format fits each situation best.
In-person clinical settings
Hospitals, urgent care centers, specialty clinics, and community health centers all represent high-demand environments for on-site medical interpretation. Surgical consultations, mental health evaluations, and pediatric appointments often require an interpreter present in the room, where physical presence and nonverbal cues carry as much weight as the spoken words themselves. In-person interpreting gives both providers and patients the fullest communication experience, particularly during emotionally sensitive or procedurally complex encounters where tone and body language shape understanding as much as vocabulary does.
On-site interpretation remains the preferred option for high-stakes encounters where immediate clarification and physical presence directly affect the quality of care.
Remote and telephonic options
Not every facility can staff on-site interpreters for every language and every shift. Video remote interpreting (VRI) connects a qualified interpreter through a secure video platform, preserving visual communication cues while reaching facilities in rural, suburban, or underserved areas. Your team can access an interpreter within minutes without coordinating travel or scheduling in advance. Telephonic interpretation works well for shorter, lower-complexity interactions, such as medication instructions, appointment scheduling, or post-discharge follow-up calls, where a phone connection covers the communication need quickly. Both remote formats extend your language access coverage across locations and shifts without requiring interpreters to be physically present at every site.

How to choose and work with an interpreter
Selecting the right interpreter directly affects the quality of every clinical encounter you facilitate for LEP patients. The medical interpreting definition makes clear that this role demands more than bilingual fluency: it requires training, ethical grounding, and familiarity with healthcare environments. Choosing someone without those qualifications, regardless of how well they speak both languages, introduces real risk into your patient communication.
Look for qualifications and training
Your first filter should be verified credentials. Look for interpreters who hold certification from recognized bodies such as the Certification Commission for Healthcare Interpreters (CCHI) or the National Board of Certification for Medical Interpreters (NBCMI). These programs test both language proficiency and medical interpreting competency, covering ethics, terminology, and protocol.
Certification signals that an interpreter has met a defined standard, not just that they happen to speak two languages.
Beyond individual credentials, work with a language services provider that vets its interpreters systematically, using ongoing quality review rather than a one-time screen. Providers with established healthcare experience, such as those holding government contracts or ATA membership, typically apply more rigorous standards than general staffing firms.
Set expectations before the appointment
Before each interpreted encounter, brief your interpreter on the subject matter and goals of the appointment. A two-minute conversation covering the patient’s presenting concern, the type of procedure being discussed, or any sensitive topics expected during the visit helps the interpreter prepare terminology and approach the session confidently.
During the appointment, speak directly to your patient, not to the interpreter. Use short, clear sentences and pause regularly to allow the interpreter to render each segment completely. This pacing reduces errors and ensures your patient receives a full, accurate message rather than a compressed summary.
Key takeaways
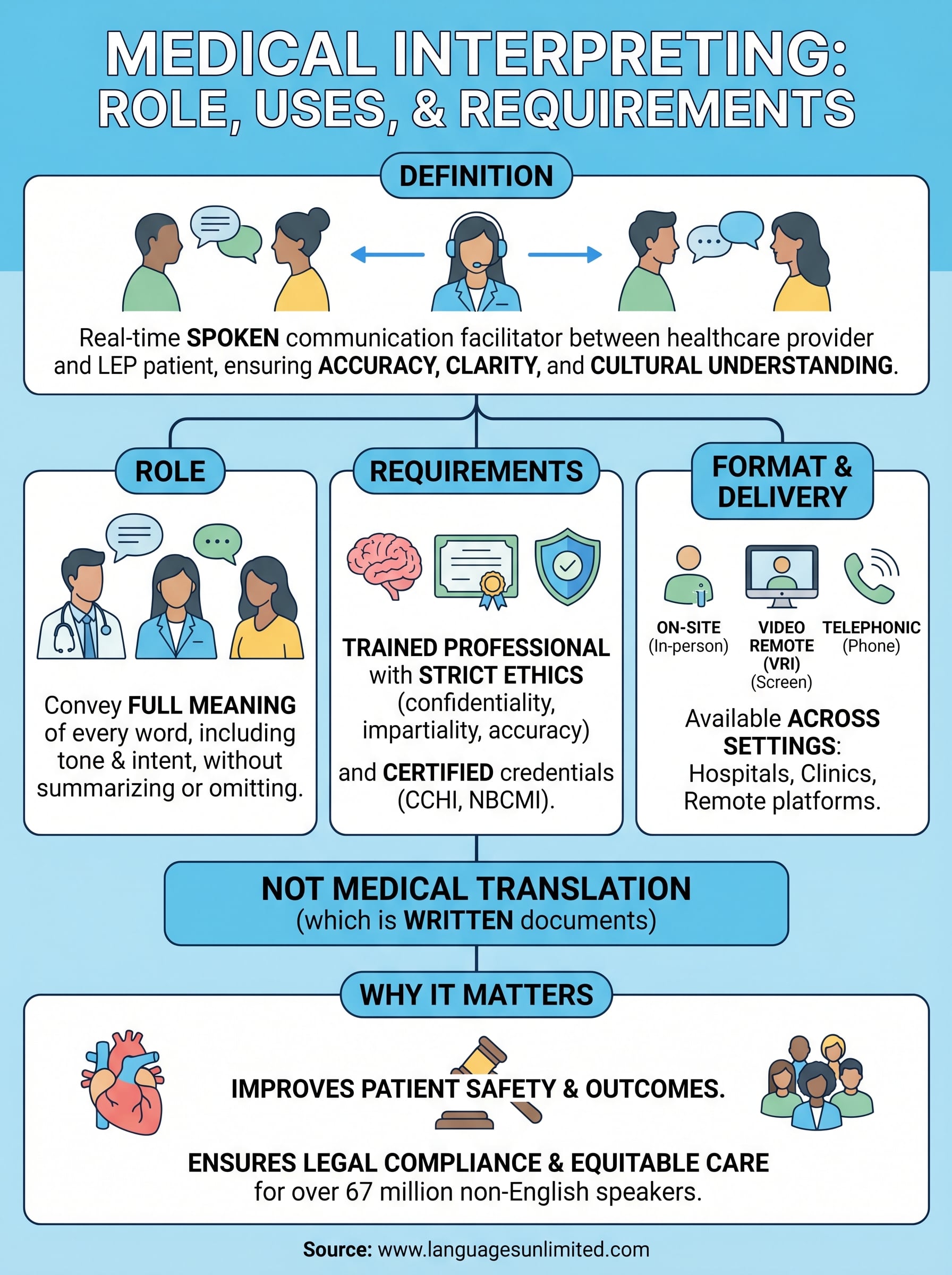
The medical interpreting definition is straightforward: a trained professional renders spoken communication in real time between a healthcare provider and a patient who speak different languages. That definition carries serious weight in practice. Your organization’s ability to serve LEP patients safely and equitably depends on using qualified interpreters, not bilingual staff or family members, across the right settings and formats.
Medical interpreting differs from translation, follows strict ethical standards, and applies across hospital floors, specialty clinics, and remote platforms. Choosing a certified interpreter and briefing them before each appointment directly improves the quality of every clinical encounter you facilitate. These are not small operational details; they are the foundation of language access done right.
If your healthcare organization needs reliable, qualified medical interpreting services across on-site, telephonic, or video remote formats, Languages Unlimited has supported facilities nationwide since 1994. Contact our team to discuss the coverage your patients need.
